Why Pulse Oximetry Is Essential for Emergency Response Teams
Emergency response teams make critical decisions in fast-moving situations. They often arrive on scene with limited background information, shifting patient status, and little time to slow down. In those moments, every tool must deliver useful information quickly and clearly. Pulse oximetry stands out because it helps responders spot trouble early, track changes in real time, and support better decisions during transport and handoff.
For emergency medical services, hospital rapid response teams, community health programs, and other healthcare professionals, pulse oximetry provides an immediate layer of clinical insight without slowing workflow. It supports patient assessment for adults, children, and infants and gives teams another way to confirm whether a patient is stable or beginning to decline. When seconds matter, that visibility can shape what happens next. Continue reading to explore why pulse oximetry is essential for emergency response teams.
Fast Insight
Emergency response rarely provides a perfect assessment environment. Lighting may be poor, and noise may interfere with communication. A patient may struggle to answer questions, or no one at the scene may know their medical history. Pulse oximetry helps cut through some of that uncertainty by providing responders with a quick point-of-care reading of oxygen saturation and pulse rate.
That matters because respiratory compromise does not always present dramatically at first. A patient can appear calm even as oxygen levels trend downward. By the time more obvious signs appear, the situation may have become harder to manage. A pulse oximeter gives teams a way to detect concerns earlier and respond with more confidence.
Better Triage
Triage depends on identifying who needs immediate attention and who can safely wait for the next level of care. Pulse oximetry supports that process by providing measurable data alongside visual assessment and patient history. It helps teams sort through presentations that may look similar on the surface but differ in severity.
Shortness of breath, chest discomfort, altered mental status, trauma, shock, and suspected infection can all require rapid prioritization. In those situations, oxygen saturation readings help crews determine how urgently a patient needs intervention or transport. The reading should never stand alone, but it strengthens clinical judgment when paired with the full picture.

A Clearer Respiratory Picture
Emergency responders often deal with airway and breathing issues before they know the full cause. A low oxygen saturation reading can point to problems linked to asthma, pneumonia, pulmonary edema, overdose, airway obstruction, or other respiratory events. Even when a patient does not describe severe breathing difficulty, pulse oximetry can reveal that oxygen delivery is under strain.
It also helps crews track whether treatment is working. When responders reposition a patient, administer oxygen, support ventilation, or begin other appropriate care, repeat readings can show whether the patient is improving, holding steady, or deteriorating. That ongoing feedback helps guide the next move instead of relying solely on first impressions.
Stronger Pediatric Support
Children and infants often present unique assessment challenges in emergency settings. They may not verbalize symptoms clearly, and subtle changes can carry more weight. Pulse oximetry gives teams a noninvasive way to gather useful data without adding significant stress to the encounter.
In neonatal and pediatric settings, device choice matters. A neonatal pulse oximeter can support more appropriate monitoring for very small patients, where fit, sensitivity, and accuracy become especially important. For teams that serve community clinics, maternal-child programs, transport units, or pediatric response settings, having the right equipment on hand can improve confidence during high-pressure calls.
More Confidence in Transport
A patient’s condition can change between first contact and arrival at the next level of care. Transport adds movement, time pressure, and environmental variables that can complicate monitoring. Pulse oximetry helps responders keep a closer watch during that phase and detect changes before they become more serious.
This insight is especially useful when a patient presents with borderline findings or when the cause of distress remains unclear. Continuous or repeated readings can show whether oxygenation remains stable during transport. That gives crews better information for destination planning, communication with receiving staff, and decisions about escalation during transport.
Valuable During Handoff
One of the most important parts of emergency response occurs at transition points. A strong handoff can help the receiving team act faster and with greater clarity. Pulse oximetry supports that handoff by providing responders with documented trends rather than a single impression.
Instead of saying a patient seemed fine at pickup but worsened en route, crews can report that oxygen saturation declined over a defined period despite supportive measures. That level of detail provides a clearer picture for emergency department teams, urgent care staff, or hospital clinicians. It also reinforces the value of consistent monitoring from scene to facility.
Useful Across Settings
Pulse oximetry is great to use across various settings. Emergency medical services use it in the field, but it also plays a role in community health programs, university clinics, urgent response teams, outpatient settings, and specialty care environments. For organizations that serve varied populations, the versatility of pulse oximetry makes it a practical investment.
That broad usefulness aligns with the needs of many professional buyers. Government agencies, nonprofits, universities, and community health centers often need tools that work across care scenarios without adding complexity. Pulse oximetry fits that need because it supports rapid assessment across many patient populations and operational settings. That’s one reason suppliers like Cascade Health Care remain relevant to professionals who need dependable diagnostic tools for real-world care settings.
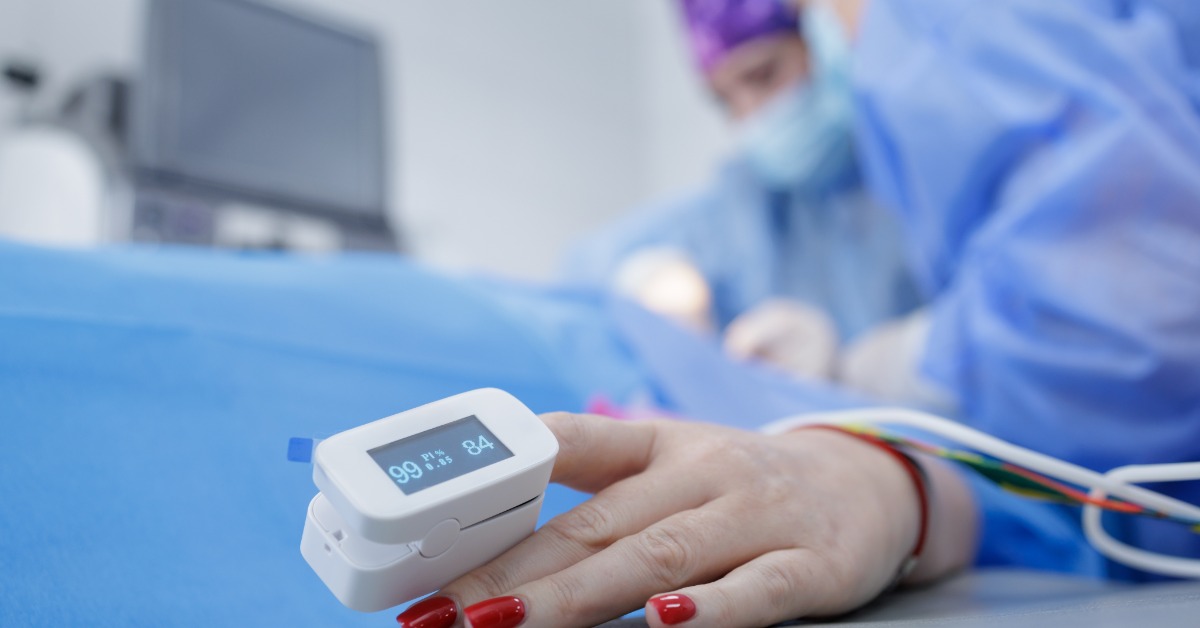
Not a Standalone Answer
Pulse oximetry matters because it provides meaningful data, not because it replaces clinical judgment. Good responders know that no single device tells the whole story. Readings can be affected by movement, poor perfusion, cold extremities, nail coverings, and other factors. Teams still need to assess work of breathing, skin signs, mental status, heart rate, history, and overall presentation.
That said, the value of pulse oximetry remains clear. It gives emergency teams another point of reference when conditions are less than ideal. It helps confirm concerns, challenge assumptions, and support decisions with objective information. In emergency response, that combination can make care more focused and more consistent.
A Smarter Equipment Choice
Emergency teams depend on tools that work under pressure. They need equipment that is simple to use, quick to apply, and easy to interpret in demanding conditions. Pulse oximetry checks those boxes for emergency response teams. It offers immediate feedback, supports ongoing monitoring, and strengthens patient assessment without creating unnecessary steps.
For professionals building emergency kits, transport bags, clinic workstations, or field response systems, pulse oximetry deserves a central place. It helps teams detect silent decline, monitor response to care, and communicate patient status more effectively from first contact through handoff. When the goal is faster recognition and better-informed action, pulse oximetry is not just helpful. It is essential.
Recent Posts
-
11 Mistakes To Avoid When Ordering Medical Supplies Online
Ordering medical supplies online can save time, simplify purchasing, and help busy teams keep essent
-
How To Choose the Right Speculum Size for Patient Comfort
A pelvic exam can feel routine for an experienced clinician, but the patient may experience it very